Partial Self-Funding Plans
Self Funded Plan Example
Self Funding 101
Most fully insured and fully self-funded employers want flexibility in making key decisions on benefits, administration and funding, yet need to limit their liability. Partial Self Funding Plans with Stop Loss Coverage for employer group health insurance, is an attractive alternative to the fully insured market for cost conscious employers. Self-funding is an alternative that enables employers to control rising healthcare costs.
A. What is a Self-Funded / Self-Insured plan?
A self-insured, or self-funded plan, is one in which the employer assumes partial financial risk for providing health care benefits to its employees. The employer decides on a plan of employee benefits, which can be similar to or identical to the employers current fully insured plan, or the employer can create whatever benefits they desire. Rather than obtaining medical coverage from an insurance carrier, the employer elects to fund the risk up to a certain level where a Reinsurance or Stop Loss Insurance carrier is brought in. The Stop Loss is designed to limit the employers loss to a specified amount, to ensure that large, or unanticipated claims, do not upset the financial integrity of a self-funded plan. The amount of risk to be insured is a function of the employers size, nature of their business, financial experience and tolerance for risk. A TPA administers the plan. Their responsibility includes maintaining eligibility, customer service, adjudicating and paying claims, preparing claim reports, plus arranging for managed care services such as network access and case management.
Usually the group medical or health plan is the focus of a self-funded program. Other benefits that are often self funded are dental, prescription drugs, vision and short term disability. Life Insurance, Accidental Death and Dismemberment and long term disability are not suitable for self-insurance.
I. Self Funding A Comparison to Fully Insured Plans
Basically, everything that is provided in a conventionally fully insured program is duplicated in the partial self funded plan. Everything that the insurance company does when it offers a conventionally insured program takes place in the partially self funded program. The difference is that with the self funded plan the employer holds the cash needed to fund benefits, and instead of sending the fully conventional premium to the insurance company, only a small fraction of the conventional premium is sent in to a reinsurance carrier. The employer purchases re-insurance for protection, holds the remainder of the conventional funds (claim funds), invests them, segregates them if desired, or uses them for general business purposes until they are needed for the funding of claims. The employer retains and keeps the funds when claims do not materialize, hence making a profit.
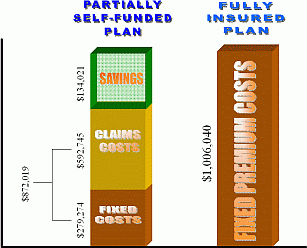
Example A: (Fully Insured Example) Acme Company is fully insured with Fully Insured Carrier and pays a premium of $1,500,000.00 annually for their health insurance plan. Claims experience shows that Acme Company only had $1,000,000 in claims and admin expenses. The fully Insured Carrier keeps $500,000 in profits.
Example B: (Self Funded Example) Acme Company's group health insurance is self funded with a Third Party Administrator with reinsurance. Acme Companys potential worst case scenario for the year is $1,600,000 annually. Acme company pays $20,000 a month in fixed premium costs and holds in claims reserves $1,360,000 for potential claims. The $1,360,000 is retained by Acme Company and it is theirs to utilize as they see fit until claims materialize. At the end of the year Acme Companys claims are $1,000,000. Acme Company retains the $360,000 it reserved in a worst case scenario. Acme Company realizes a $260,000 savings by going Self Funded versus Fully insured.
The employer is protected by three facets of insurance protection, the specific deductible or (Specific Stop Loss) which protects against any one person claims exceeding a specified amount, the integrated aggregate which protects against any excess monthly claims (so the employer may budget and allocate only the conventional equivalent premium each month, then not have to worry about an adverse month when more than usual claims are presented), and an annual aggregate reinsurance to protect against claims greater than the conventional equivalent.
II. WHAT ARE THE ADVANTAGES OF SELF FUNDING?
The advantages of self-funding are many. There is tremendous flexibility in the benefit plan design. You can decide what you want to cover and what you don't, whether it's certain vaccinations, chiropractors, injectibles, obesity, or infertility.
Another major advantage, is portability from one carrier to another. "There's no disruption in plan when you shift between reinsurance carriers. You don't have to start all over again with new I.D. cards, booklets and doctors, the way you do with the fully-funded plans."
Also, for employers with more than one office, it is possible to offer the same plan to everyone in every location. This makes it so much more administratively simple. By Self Funding an employer can utilize one national network or multiple local PPO networks with the same benefit plans.
But the bottom line, is cost savings. If you have a good expected claims year, that is the best scenario. But even if you don't, there's maximum liability in place.
Another advantage of Self Funding is the ability to class out the executives and provide them with a 100% benefit where, executives and their families pay no copays, deductibles or coinsurance.
A. Immediate Benefits and Advantages of Self Funding
1. Fully Insured Carriers Profit Margin:
A fully insured carriers profit margin can be as high as 52% with your current fully insured health plan. This means if your premium is $1 million, the insurance carriers Profit can be as high as $520,000.
Note: Even with a highly profitable employer case a fully insured carrier will have no problem hitting the employer with a double digit rate increase. Insurance carriers continually base rate increases upon a concept called pooling. Pooling says that if other employers the carrier insures had bad claims experience, which hurt profitability, the fully insured carrier will penalize and raise rates for all employers. Other fictitious reasons fully insured carriers will give for rate increases is trend. Trend means increases in the healthcare industry. The fully insured carrier will argue a double digit increase was justified by "trend" on an employer who is running at 50% of claims (highly profitable). This means even though that particular employer has excellent claims experience and is not running at "trend" where other companies have bad experience, the carrier will still raise their rates.
2. Elimination of Premium Tax:
In most states there is no premium tax for self funded plans. This results in an immediate savings since between 2%-4% of your current fully insured health plans costs a premium taxes.
3. Improved Cash Flow:
Moving from a fully insured plan to a self funded plan usually results in about 3 months of relatively little new claims. During this time, the previous fully insured carrier is still paying claims incurred prior to the new self funded plan year. This claims lag allows your new Self Funded plan the opportunity to build and establish a reserve to pay future claims.
Also, reserves for claims are held by the employer and only released if claims materialize, resulting in an improved cash flow for the employer.
4. Control & Flexibility of Plan Design Benefits:
The employer can duplicate its current fully insured benefit plan or it can redesign and tailor the benefits to meet the specific needs of the employer. This means the employer can eliminate benefits which result in plan abuses or high utilization. The employer can also create special executive benefits.
5. Eliminate State Mandated Benefits:
Since Self funded plans are governed by ERISA, they follow Federal law, and are not required to cover State-Mandated benefits, which can be expensive and unnecessary. By eliminating unnecessary and expensive state mandated benefits employers can realize an immediate savings. Employers can also set the limits on certain benefits, where with a fully insured plan there may be state required limits. Since fully insured plans include state mandated benefits the cost of offering these benefits raises the costs of the health plan to the employer.
6. Control of Reserves Return of Investment on Reserves:
A good portion of your fully insured premium is held by the fully insured carrier as a state required reserve for claims and inflation. Under Self Funding the employer maintains and controls reserves and can invest these or put them in an interest bearing account. The employer retains the reserves when claims do not materialize, and there are no restrictions on reserves with a self funded plan..
7. Claims Experience Immediate Realization of Hard Dollar Savings:
Under a fully insured program, if an employers experience is better than expected, the insurance company gains financially and makes an unexpected profit. The insurance carrier does not refund the excess profit to the employer.
Even if an employer had good experience, the insurance company will still pass on a renewal based upon the insurance companies pool of thousands of groups. You are not truly rated based upon your claims experience and can be treated unfairly.
With Self Funding your renewals are based on YOUR companies claims experiences, and it is not based on thousands of other companies that have no relation to your company or industry. You, the Employer, not the insurance company enjoy the advantage of favorable claims experience. You, the Employer, keep the savings.
B. OTHER IMPORTANT ADVANTAGES
1) Improved Employee Satisfaction- Personalized Employee Service:,
Third Party Administrators specialize in one thing, Customer Service. Their sole purpose is to provide the best quality service possible, and to personalize that service to members. This includes dedicated account representatives who know not only the employers account but the individual employees of each company. Employees and HR get on a first name basis with claims examiners, and are not transferred to a random person that does not know anything of the employee or the employer.
2) Lower Costs of Operation:
Third Party Administrators have lower overhead and expenses than a fully insured plan, which result in an immediate direct savings for the employer, when switching to Self Funding.
3) Claim Utilization and Cost Controls:
Third Party Administrators review utilization of the plan and benefits and see where the employers claims and costs are. This allows the employer along with the TPA to make informed decisions as to plan benefits, costs, and any adjustments that need to be made. TPAs also implement unique programs such as hospital bill auditing, case management, pre-certification review, lab programs, etc to keep costs down.
C. NATIONAL OR REGIONAL COMPANIES & PROVIDER NETWORKS
The fully insured, insurance companys inflexibility to deal with national or regional employers means a multi-location employer cannot offer the same benefits or insurance carrier options to all of its employees. Some mutli-location employers have to use multiple fully insured carriers with varying benefit plan designs. This results in far higher plan management costs, and extra administrative work for human
With a self-funded plan, a multi-location employer can choose from one network to dozens of networks, offering a single standard benefit plan design across several states with significant savings on plan management expenses.
This saves your human resource department from dealing with multiple confusing health plan designs and multiple insurance carriers.
D. PRESCRIPTION DRUGS
With rising prescription drug costs it can be unnerving that an average employers prescription drug plan can be the cause of almost 25% of the cost of the companys group health plan. Fully Insured carriers pass along minimal prescription drug discounts to employers and keep any pharmaceutical rebates. The result is larger Rx costs and claims experience, which then result in higher rate increases.
With a Self Funded Plan, Employers will actually receive substantial rebates ($ money back each quarter from pharmaceutical managers). Companys will also receive the strongest prescription drug discounts (depends on the TPA) in the country, reducing the employers prescription drug costs, and hence resulting in lower costs for the group health plan.
E. PERCEIVED DISADVANTAGES of Self Funding
Question: Won't my own poor current claims experience means that the plan will be costly?
Answer: Poor claims can affect costs, this is true, but they will be less costly than a fully insured plan, as you are not paying for taxes and profit in addition to insurance coverage.
Question: Will budgeting the Plan be difficult?
Answer: Prior claims experience guides your financial commitment, and stop-loss insurance guarantees performance.
Question: Will termination of the Plan be difficult if we find it necessary?
Answer: Stop loss coverage is structured to pick up claims incurred in, but reported after plan year.
Question: Is there added fiduciary and legal responsibility?
Answer: The professional administrator provides advice and guidance, whenever help is needed.
For information about IMA and the companys approach to designing cost-effective self-funded health insurance programs, please complete the form on the contact page.
For a separate article titled; Self-Funding An Overview & Explanation of Misconceptions, written by Frederick D. Hunt, Jr., SPBA President, click here
